Pharmaceutical Rep Whistleblower Warned of the Dangers of Antipsychotic Drug Seroquel
 By the C|C Whistleblower Lawyer Team
The Chicago Tribune reports on the story of pharmaceutical sales representative turned whistleblower, Allison Zayas. Zayas worked for pharmaceutical company AstraZeneca marketing and selling the antipsychotic drug Seroquel to doctors and nursing homes. In the winter of 2009, one of Zayas’ clients, a doctor, described to her how a patient died while taking a combination of...
By the C|C Whistleblower Lawyer Team
The Chicago Tribune reports on the story of pharmaceutical sales representative turned whistleblower, Allison Zayas. Zayas worked for pharmaceutical company AstraZeneca marketing and selling the antipsychotic drug Seroquel to doctors and nursing homes. In the winter of 2009, one of Zayas’ clients, a doctor, described to her how a patient died while taking a combination of...
 By the C|C Whistleblower Lawyer Team
DaVita Rx LLC, a nationwide pharmacy that specializes in serving patients with severe kidney disease, agreed to pay a total of $63.7 million to resolve False Claims Act allegations relating to improper billing practices and unlawful financial inducements to federal healthcare program beneficiaries, the Justice Department announced today. DaVita Rx is based in Coppell,...
By the C|C Whistleblower Lawyer Team
DaVita Rx LLC, a nationwide pharmacy that specializes in serving patients with severe kidney disease, agreed to pay a total of $63.7 million to resolve False Claims Act allegations relating to improper billing practices and unlawful financial inducements to federal healthcare program beneficiaries, the Justice Department announced today. DaVita Rx is based in Coppell,...
 By the C|C Whistleblower Lawyer Team
AmerisourceBergen, a Pennsylvania-based company that provides drug distribution and related services, has agreed to
By the C|C Whistleblower Lawyer Team
AmerisourceBergen, a Pennsylvania-based company that provides drug distribution and related services, has agreed to  By the C|C Whistleblower Lawyer Team
The founder and majority owner of Insys Therapeutics Inc., was arrested and charged with leading a nationwide conspiracy to profit by using bribes and fraud to cause the illegal distribution of a Fentanyl spray intended for cancer patients experiencing breakthrough pain.
"More than 20,000 Americans died of synthetic opioid overdoses last year, and millions are addicted to...
By the C|C Whistleblower Lawyer Team
The founder and majority owner of Insys Therapeutics Inc., was arrested and charged with leading a nationwide conspiracy to profit by using bribes and fraud to cause the illegal distribution of a Fentanyl spray intended for cancer patients experiencing breakthrough pain.
"More than 20,000 Americans died of synthetic opioid overdoses last year, and millions are addicted to...
 By the C|C Whistleblower Lawyer Team
On Tuesday, 38-year-old Joseph Baumiller of Dallas, Texas pleaded guilty to one count of conspiracy to defraud TRICARE, the health care program serving military members and their families. Baumiller, the former president of Trilogy Pharmacy, admitted to conspiring with several marketers, physicians, and other pharmacists to orchestrate a scheme involving the payment of kickbacks...
By the C|C Whistleblower Lawyer Team
On Tuesday, 38-year-old Joseph Baumiller of Dallas, Texas pleaded guilty to one count of conspiracy to defraud TRICARE, the health care program serving military members and their families. Baumiller, the former president of Trilogy Pharmacy, admitted to conspiring with several marketers, physicians, and other pharmacists to orchestrate a scheme involving the payment of kickbacks...
 By the C|C Whistleblower Lawyer Team
As
By the C|C Whistleblower Lawyer Team
As 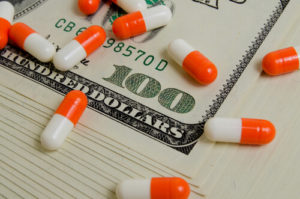 Aegerion Pharmaceuticals will plead guilty to charges concerning its prescription drug, Juxtapid, the Department of Justice announced on Friday. According to the Justice Department’s press release:
Aegerion introduced Juxtapid into interstate commerce that was misbranded because, among other things, Aegerion failed to comply with a Risk Evaluation and Mitigation Strategy (REMS). The resolution also...
Aegerion Pharmaceuticals will plead guilty to charges concerning its prescription drug, Juxtapid, the Department of Justice announced on Friday. According to the Justice Department’s press release:
Aegerion introduced Juxtapid into interstate commerce that was misbranded because, among other things, Aegerion failed to comply with a Risk Evaluation and Mitigation Strategy (REMS). The resolution also...
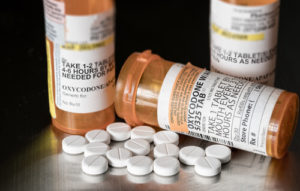 By the C|C Whistleblower Lawyer Team
An article in the
By the C|C Whistleblower Lawyer Team
An article in the  By the C|C Whistleblower Lawyer Team
This week's Department of Justice "Catch of the Week" goes to Novo Nordisk Inc. On Tuesday, the company agreed to pay $58.65 million to settle charges it violated the
By the C|C Whistleblower Lawyer Team
This week's Department of Justice "Catch of the Week" goes to Novo Nordisk Inc. On Tuesday, the company agreed to pay $58.65 million to settle charges it violated the 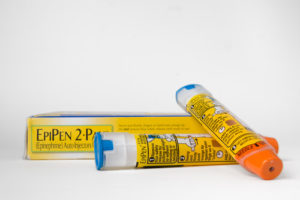 By the C|C Whistleblower Lawyer Team
Last Friday, the Department of Justice (“DOJ”)
By the C|C Whistleblower Lawyer Team
Last Friday, the Department of Justice (“DOJ”)